Drug Interactions Explained
In the field of modern pharmacology, the interaction between different chemical substances within the human body is a critical area of clinical concern. A drug interaction occurs when the effect of a particular medication is altered by the presence of another drug, a specific food item, or even an underlying medical condition. At Mediquickinfo, we recognize that as “Polypharmacy”—the use of multiple medications—becomes more common, the risk of dangerous interactions increases exponentially. These interactions can lead to reduced efficacy of treatment, unexpected side effects, or severe toxic reactions. This 2000+ word comprehensive guide provides a clinical explanation of how drug interactions manifest, the biological pathways involved, and evidence-based strategies for minimizing pharmacological risk.
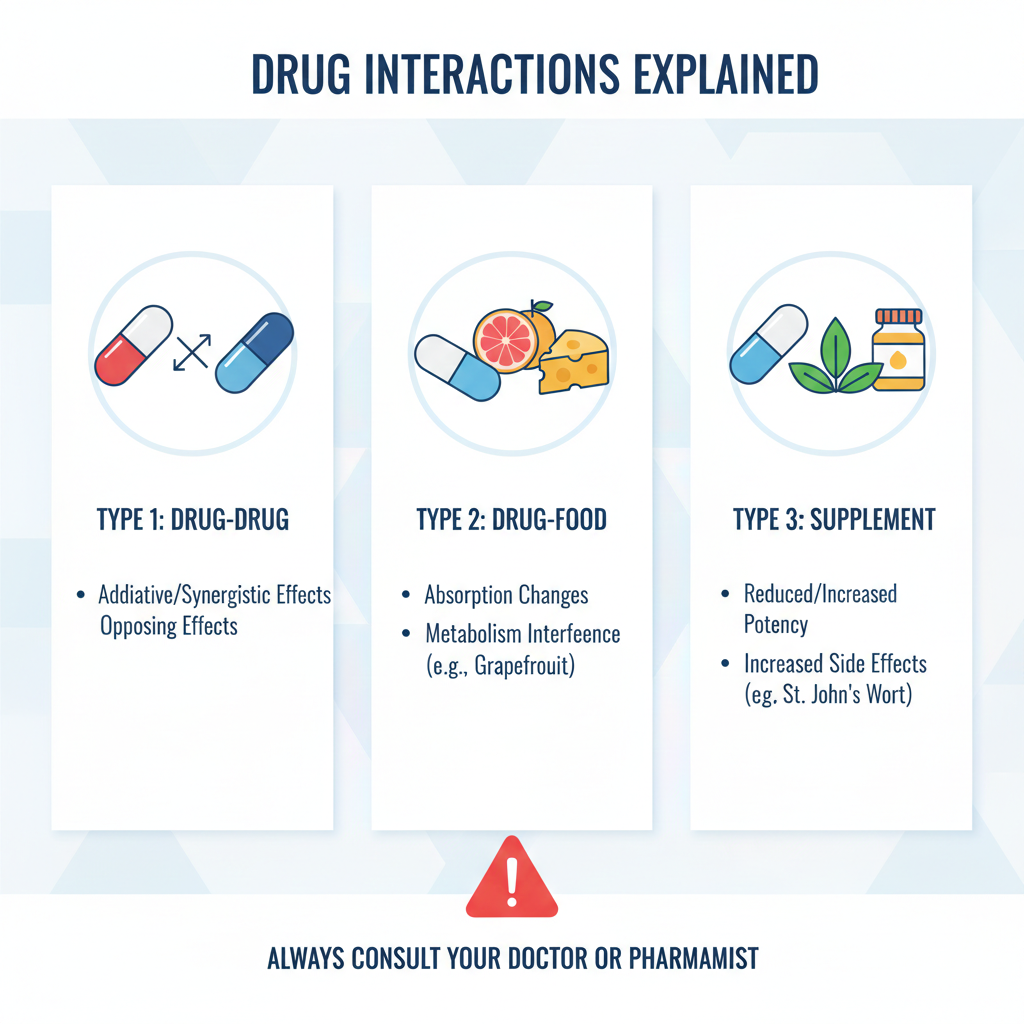
1. The Two Main Types: Pharmacokinetic vs. Pharmacodynamic
From a clinical perspective, drug-drug interactions are broadly classified into two categories. **Pharmacokinetic interactions** occur when one drug affects how another is absorbed, distributed, metabolized, or excreted (ADME). For example, a drug might inhibit a specific liver enzyme (like the cytochrome P450 system) that is responsible for breaking down another medication. At Mediquickinfo, we analyze how this leads to an accumulation of the second drug in the bloodstream, potentially reaching toxic levels. Conversely, some drugs act as “inducers,” speeding up the metabolism of others and rendering them ineffective.
**Pharmacodynamic interactions** occur when two drugs have similar or opposing physiological effects on the same biological receptor or organ system. These can be “Additive” (1+1=2), “Synergistic” (1+1=3), or “Antagonistic” (1+1=0). A classic clinical example is the combination of alcohol with benzodiazepines; both are central nervous system depressants. Taking them together does not just double the effect; it creates a synergistic respiratory depression that can be fatal. Understanding these biological pathways is the foundation of medication safety protocols at Mediquickinfo.
2. Drug-Food and Drug-Supplement Interactions
It is a common misconception that interactions only occur between prescription pills. At Mediquickinfo, we stress that what you eat and the supplements you take can drastically alter your medication’s performance. The “Grapefruit Effect” is perhaps the most famous; grapefruit contains furanocoumarins that block intestinal enzymes, allowing too much of certain heart and blood pressure drugs to enter the blood. Similarly, high-vitamin K foods (like spinach or kale) can interfere with the blood-thinning effects of Warfarin, requiring careful dietary consistency.
Herbal supplements are another high-risk area. St. John’s Wort is a potent enzyme inducer that can reduce the blood levels of critical medications, including anti-rejection drugs for transplant patients and hormonal contraceptives. At Mediquickinfo, we advocate for a “Total Substance Inventory”—always informing your clinician about every tea, vitamin, and herbal extract you consume. The chemical complexity of natural supplements does not make them “safer” when combined with synthetic pharmacology.
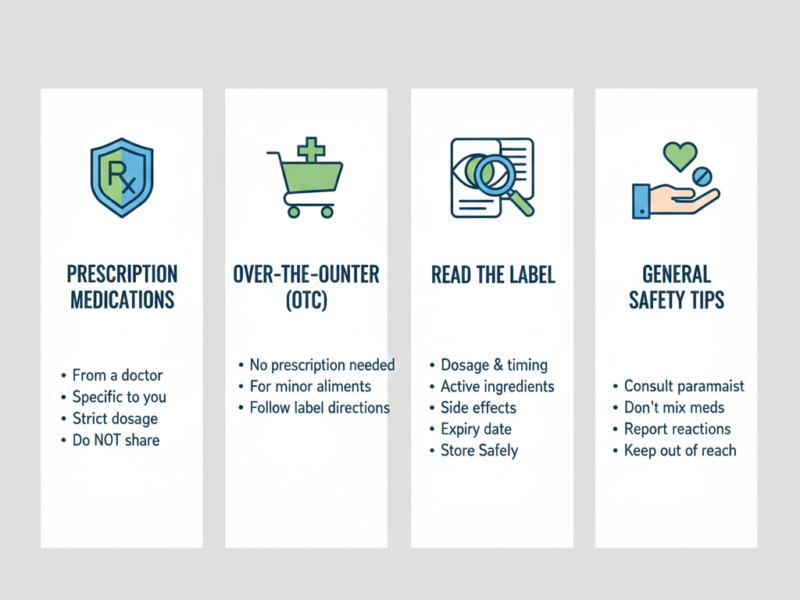
3. The Clinical Risk of Over-the-Counter (OTC) Drugs
Many patients assume that because a drug is available without a prescription, it is free of serious interaction risks. Mediquickinfo clinical data warns that common OTC medications like NSAIDs (Ibuprofen or Naproxen) can have dangerous interactions with prescription blood pressure medications (ACE inhibitors) and diuretics. This combination, often called the “Triple Whammy,” can cause acute kidney injury by disrupting the delicate pressure balance within the renal filtration system.
4. Preventive Strategies: Safeguarding Your Health
Preventing drug interactions requires a proactive and informed approach. At Mediquickinfo, we recommend the use of a single pharmacy for all your prescriptions, as their software can automatically flag potential interactions. Maintaining an up-to-date medication list, including dosages and reasons for use, is essential. Furthermore, never start a new supplement or OTC drug without consulting a pharmacist if you are on chronic medication. Clinical awareness of your body’s response—such as sudden dizziness, rashes, or digestive changes after adding a new drug—is a vital early warning system.
Conclusion: Knowledge as Your Best Defense
Drug interactions are a complex but manageable aspect of modern medicine. By understanding the clinical mechanisms of how substances conflict or combine within your body, you can take control of your pharmacological safety. At Mediquickinfo, we believe that health literacy is the ultimate protection against medication errors. Your treatment plan should be a harmonious synergy, not a chemical battleground. Trust Mediquickinfo for the clinical literacy you need to navigate your health journey with precision and confidence. Safety starts with an informed mind.